Table of Content
You’ve Been Told It’s All About Testosterone—But Is It?
You know that sinking feeling when you realize you haven’t even thought about sex in weeks?
When your partner makes a move and your first reaction isn’t desire — it’s anxiety about whether you’ll even be able to respond?
Every commercial, every men’s health article, every conversation at the gym points to the same culprit: low testosterone.
“Get your T checked,” they say. “It’s just your hormones,” they promise.
But here’s what nobody tells you: the relationship between testosterone and libido is way more complicated than the testosterone industry wants you to believe.
The Myth vs. Reality of “Low T”
The testosterone replacement therapy market is worth billions of dollars for a reason.
They’ve convinced an entire generation of men that declining libido equals low testosterone, and low testosterone equals an easy fix with a simple injection or gel.
The reality is much more nuanced.
Yes, testosterone plays a crucial role in your sex drive. But it’s not the simple on/off switch you’ve been told it is.
Think of testosterone like the engine in your car. It’s essential, but if your fuel tank is empty (sleep), your battery is dead (stress), or your transmission is broken (relationship issues), even the best engine won’t get you moving.
So before you assume your libido problems are all about testosterone, let’s look at what the science actually says.
How Testosterone Actually Affects Your Sex Drive
Let’s start with what we know for certain.
The Science Behind Hormones and Desire
Testosterone is your primary sex hormone. Research confirms that it directly influences sexual thoughts, desire, and the frequency of sexual activity.
But here’s where it gets interesting: there’s no perfect testosterone level that guarantees a strong libido.
Some men with testosterone levels on the lower end of “normal” have robust sex drives. Others with levels in the upper normal range struggle with desire.
Why? Because testosterone doesn’t work alone.
The libido equation includes:
- Testosterone (the foundation)
- Dopamine (the motivation neurotransmitter)
- Nitric oxide (for physical arousal)
- Psychological factors (stress, confidence, attraction)
- Physical health (cardiovascular, metabolic)
- Sleep quality (when testosterone is actually produced)
Why It’s More Complex Than You Think
Here’s the thing most doctors won’t tell you: the relationship between testosterone and libido isn’t linear.
Studies show that there’s a “threshold effect”: below approximately 300 ng/dL, most men experience declines in libido and sexual function, whereas above that level, additional increases in testosterone don’t necessarily boost sex drive further—it behaves more like a light switch than a dimmer.
It’s like a light switch, not a dimmer.
Once you have “enough” testosterone, other factors become much more important for your actual desire and performance.
This explains why:
- Some men on testosterone therapy still have libido issues
- Natural testosterone boosters often disappoint
- Fixing sleep or stress can improve libido faster than hormones
- Relationship quality strongly predicts sexual satisfaction
The bottom line? Testosterone is necessary but not sufficient for a healthy sex drive.
The Normal Decline vs. Real Problems
Let’s get real about what happens as you age.
What Happens After 35 (And Why It’s Normal)
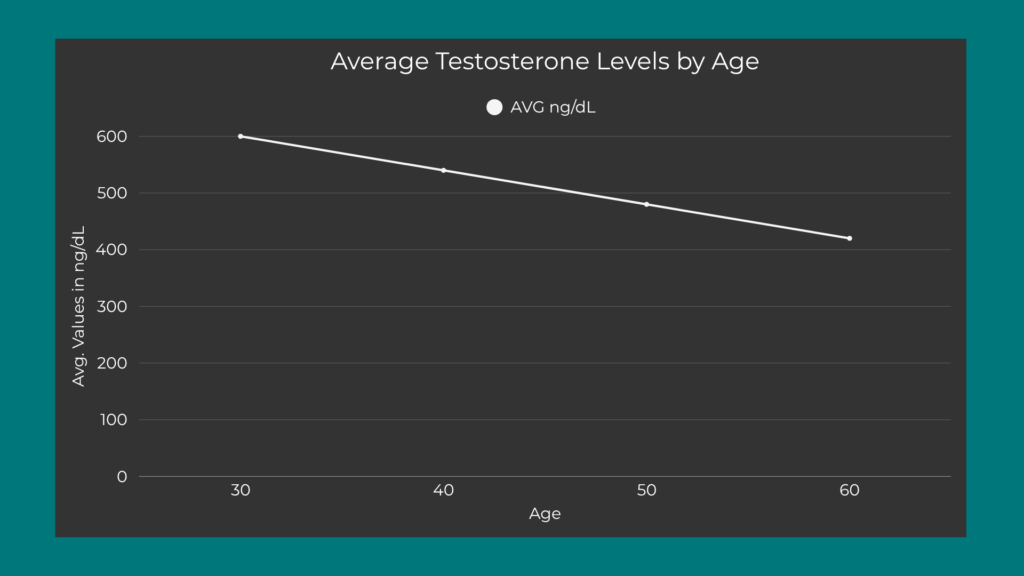
Starting around age 30, your testosterone naturally declines at a rate of approximately 1% per year. Longitudinal research supports this consistent decline—while not drastic annually, it’s a predictable part of aging and doesn’t necessarily lead to problems unless levels drop significantly.
The math:
- At 30: Average 600 ng/dL
- At 40: Average 540 ng/dL
- At 50: Average 480 ng/dL
- At 60: Average 420 ng/dL
Most men don’t notice significant libido changes until their 40s or 50s, when the cumulative effect becomes more apparent.
But here’s what’s crucial: this decline is often gradual enough that your body adapts.
The guys who struggle most aren’t necessarily those with the lowest testosterone. They’re often the ones whose levels dropped quickly due to:
- Chronic stress
- Poor sleep for extended periods
- Significant weight gain
- Certain medications
- Underlying health conditions
When Low Testosterone Becomes a Concern
So when should you actually worry about your testosterone levels?
Clear warning signs:
- Total testosterone below 300 ng/dL on multiple tests
- Sudden, dramatic decline (not gradual aging)
- Multiple symptoms beyond just libido (fatigue, muscle loss, mood changes)
- Inability to maintain erections even when desire is present
The gray zone (300-500 ng/dL): This is where most men fall, and it’s where the real confusion happens. You might have symptoms, but you’re technically “normal.”
Here’s the reality: if you feel terrible and your testosterone is 350, that might be low for you, even if it’s “normal” for the average population.
Signs Your Testosterone Is Actually Affecting Your Libido
Not every low libido case is about testosterone. Here’s how to tell if hormones are actually the issue.
Physical Symptoms That Matter
Strong indicators testosterone is involved:
- Difficulty getting or maintaining erections
- Reduced morning erections (you used to wake up ready to go)
- Longer recovery time between sexual activities
- Decreased sensitivity during intimate moments
- Physical fatigue that doesn’t improve with rest
Other physical changes:
- Muscle mass loss despite staying active
- Increased body fat, especially around the midsection
- Thinning hair or changes in body hair patterns
- Hot flashes or night sweats (yes, men get these too)
Mental and Emotional Changes
Psychological symptoms often linked to low testosterone:
- Decreased motivation for sex (not just opportunity)
- Reduced sexual fantasies or thoughts
- Loss of confidence in sexual situations
- Feeling like you’ve lost your “masculine edge”
- Depression or persistent low mood
But here’s the crucial distinction: these symptoms can also be caused by stress, sleep deprivation, relationship issues, or other health problems.
The key is looking at the pattern and timing of these changes.
Beyond Testosterone: Other Factors Killing Your Drive
Here’s where most men get it wrong. They assume low libido equals low testosterone and miss the real culprits.
The Hidden Culprits Most Men Miss

Sleep deprivation: Research shows that restricting sleep to less than 5 hours per night for a week can reduce testosterone levels in healthy young men by 10–15%—equivalent to the hormonal impact of aging a decade. But sleep affects libido in other ways too — it impacts mood, energy, and stress hormones.
Chronic stress: Cortisol, your stress hormone, directly suppresses testosterone production. But stress also kills libido independently by making your brain prioritize survival over reproduction.
Medications: SSRIs, blood pressure medications, and even some allergy meds can crush libido without affecting testosterone at all.
Relationship issues: You can have sky-high testosterone, but if you’re angry, disconnected, or anxious with your partner, desire disappears.
Poor cardiovascular health: Erections require good blood flow. Heart disease, diabetes, and high blood pressure affect performance regardless of hormone levels.
Why Testosterone Replacement Isn’t Always the Answer
Here’s a hard truth: testosterone therapy works great for men who actually have low testosterone. For everyone else, it’s often disappointing.
The men who benefit most from testosterone replacement are those with:
- Clearly low levels (under 300 ng/dL)
- Multiple symptoms beyond just libido
- No other obvious causes for their symptoms
- Realistic expectations about outcomes
Common disappointments with testosterone therapy:
- Libido improves but relationship issues remain
- Physical symptoms improve but psychological factors don’t
- Initial boost that plateaus after a few months
- Side effects that outweigh benefits
The bottom line: fix the fixable factors first before assuming you need hormones.
What You Can Actually Do About It
Ready for some good news? Most libido issues are fixable without injections or gels.
Natural Ways to Support Healthy Testosterone
Sleep optimization (the biggest bang for your buck):
- Aim for 7–9 hours of quality sleep consistently
- Keep your bedroom cool (around 65–68 °F) and dark
- Avoid screens for at least an hour before bed
Studies confirm that improving sleep quality and duration can significantly support testosterone production—especially deep stages like REM and slow-wave sleep, where testosterone naturally rises during the night
Strength training:
- Lift heavy weights 2-3 times per week
- Focus on compound movements (squats, deadlifts, presses)
- Keep sessions under 60 minutes to avoid excessive cortisol
Research demonstrates consistent resistance training—particularly free‑weight, large‑muscle group workouts—elicits acute increases in testosterone and supports longer‑term hormonal adaptation.
Stress management:
- Practice daily stress reduction (meditation, deep breathing, yoga)
- Set boundaries around work and technology
- Address relationship conflicts directly
- Consider therapy for chronic stress or anxiety
Nutrition for hormone health:
- Maintain a healthy body weight (excess fat converts testosterone to estrogen)
- Eat adequate healthy fats (20-35% of calories)
- Don’t severely restrict calories for extended periods
- Consider vitamin D supplementation if deficient
When to Consider Medical Intervention
See a doctor if:
- Your total testosterone is below 300 ng/dL on multiple morning tests
- You have multiple symptoms that significantly impact your quality of life
- Natural approaches haven’t helped after 3-6 months of consistent effort
- You suspect an underlying medical condition
What to expect from testosterone therapy:
- Gradual improvement over 3-6 months (not immediate)
- Better energy and mood often come before libido improvements
- Regular monitoring of blood levels and side effects
- Potential risks including sleep apnea, blood clots, and prostate issues
Alternative medical approaches:
- Clomiphene citrate (stimulates natural testosterone production)
- HCG therapy (preserves natural hormone production)
- Addressing underlying conditions (sleep apnea, diabetes, thyroid issues)
- Medication adjustments if current drugs are affecting libido
Frequently Asked Questions About Testosterone and Libido
Q: At what age does testosterone start affecting libido? A: Testosterone begins declining around age 30 by 1% yearly, but most men don’t notice libido changes until their 40s when cumulative effects become apparent.
Q: Can you have normal testosterone but still have low libido? A: Yes. Stress, sleep issues, medications, and relationship factors can suppress libido even with normal testosterone levels.
Q: How quickly does testosterone therapy improve sex drive? A: Most men see libido improvements within 3-6 weeks of starting therapy, with peak benefits typically reached after 3-6 months.
Q: Are there natural ways to boost testosterone for libido? A: Absolutely. Strength training, quality sleep, stress management, and proper nutrition can significantly improve testosterone and libido naturally.
The Bottom Line
The relationship between testosterone and libido isn’t the simple equation you’ve been sold.
Yes, testosterone matters. It’s the foundation of male sexual desire. But it’s not the magic bullet that fixes every libido problem.
Here’s what you need to understand:
Most men with libido issues don’t have severely low testosterone. They have normal-ish levels that are being undermined by stress, poor sleep, relationship problems, or health issues.
The men who get their sex drive back aren’t necessarily the ones who get testosterone injections. They’re the ones who take a comprehensive approach to their health and relationships.
Your action plan:
- Get your testosterone tested (morning, fasted, multiple times)
- Address sleep, stress, and relationship factors first
- Give natural approaches 3-6 months of consistent effort
- Consider medical intervention if levels are clearly low or natural approaches fail
- Remember that libido is about more than just hormones
If this resonated with you, start with the basics: better sleep, regular exercise, and honest communication with your partner. These changes often work faster and more effectively than any hormone therapy.
Your libido — and your overall vitality — depends on treating your body and mind as the complex system they are, not looking for simple solutions to complicated problems.
Disclaimer: This content is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.